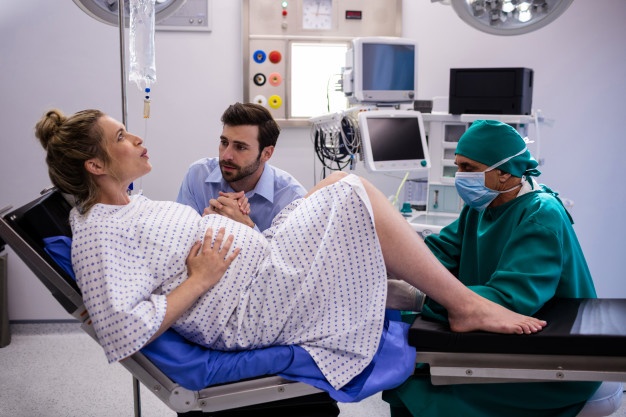
Induction of Labour: Your Body, Your Decisions
With induction rates running at around 40% in some hospitals, chances are that as you reach the end of your pregnancy you’ll be offered an induction for one reason or another. The law says that the only person who can make the decision about whether or not to accept induction is the person whose body it is so even if you’re told that you’ll be booked for an induction, or that you ‘have to’ be induced, the decision is still yours!
If you choose to decline induction you don’t need to justify this decision, or persuade anyone that it’s what you want to do. This is because no one has the right to force you to have one, they can only offer. They are not allowed to try to coerce you, or threaten you and you can report anyone who does this to the hospital. You don’t need to fight, you can simply say “I have made the decision to not have an induction, thank you”. In fact, the NICE Guideline on Induction of Labour specifically states, “If a woman chooses not to have induction of labour, her decision should be respected.” (reference: https://www.nice.org.uk/guidance/cg70/chapter/1-Guidance#information-and-decision-making – 1.2.1.3)
If you later decide that you have changed your mind, and you want to go ahead with the induction, you can simply contact your midwife who will book it for you.
If you are being offered an induction because you’re heading towards 42 weeks of pregnancy there are some important things to know.
There is strong evidence that stillbirth rates LOWER after 42 weeks!
We know, this is exactly the opposite to what is currently believed. This is because most research that was done into stillbirth at around this stage of pregnancy showed a very slight increase in stillbirth rates after 41 and 42 weeks. This research, as is the case with most studies, looked at a limited group of pregnant women and people rather than every pregnant woman and person (because this is usually almost impossible to do when doing research) and then making an educated guess that the results would be the same if everyone had been included in the study.
Unusually, it turns out that we do have the data on ‘everyone’ when it comes to stillbirth because it’s recorded by an organisation called MBBRACE. Therefore, we don’t need to reply on studies which look at a smaller group of people and hope that this data applies to everyone.
When we look at all of the stillbirths in the UK for the last ten years – millions of pregnancies – we find that in fact the stillbirth rate goes down after 42 weeks! It is important to know that it is likely that most babies who were considered to be at risk in some way other than simply length of pregnancy are likely to have been born by induction or caesarean before 42 weeks, but this leaves pregnant women and people who have no other medical concerns who are going on to have longer pregnancies without an increase – in fact a decrease – of the risk of stillbirth.
You can read more about this surprising data on the AIMS website.

NICE Guidelines support the choice to not be induced
The NICE Guidelines linked above state that ‘expectant management’ is as valid an option at 41 or 42 weeks as being induced. This includes offering two appointments a week for the baby to be monitored and checked, but this is not obligatory. Induction is simply one option of several available to you.
Caesarean is another option!
If you are reaching the end of pregnancy and don’t want to wait for spontaneous labour for any reason, induction isn’t the only option. If there is a medical reason that your pregnancy should end before labour starts on its own, induction is often the only thing that’s offered, but you can ask for a caesarean if you would prefer. Your rights to choose a caesarean are detailed in the AIMS Guide to Your Rights in Pregnancy and Birth.
If you choose induction, you can choose your options
Take a look at our article on your decisions during induction, because it’s really important to know that you have choices all the way through if you make the decision to be induced!
‘Due dates’ are really just a guess
Our ‘due date’ is set at the day we reach 40 weeks of pregnancy. This is entirely made up and has no scientific validity. It is just a date that is somewhere between the most common time to give birth – between 37 and 42 weeks. The due date could have been set at 41 weeks, or 40 weeks and 3 days and mean exactly the same thing (nothing!).
We are not overdue once we’re over 40 weeks, we’re simply pregnant for longer than 40 weeks, just as the week before we were pregnant for longer than 39 weeks.
In summary
The options that you have if your pregnancy lasts longer than average is to simply wait for spontaneous labour, wait for labour but have your baby monitored a couple of times a week, be induced or have a caesarean. If you decide to decline the offer of induction but later change your mind, you can do so.
Induction is a serious medical intervention, but that doesn’t mean that the doctors and the hospital take over your body and your rights to decide. You can choose whether or not you wish to have an induction and you don’t need to persuade anyone else to agree with you! Any medical intervention is an offer – no matter how it’s presented to you – and the only person who can decide whether or not to go ahead with it is you.

Leave A Comment